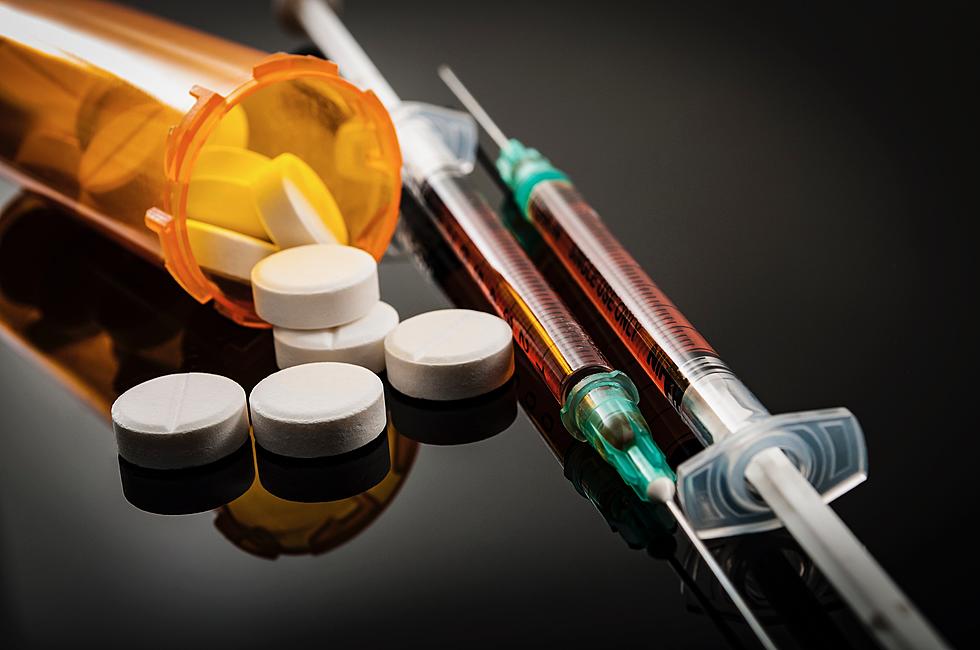
Chronic pain sufferers: Stop treating us all like addicts!
Atlantic County resident Ron Dase ran his own business, but several years ago he developed medical issues, nerve problems and was forced to have several surgeries.
“One of the surgeries went horribly wrong and I’ve been really messed up pain-wise ever since then,” he said.
As a result, Dase has been on several medications, including Oxycontin and Percocet, for more than a decade.
It took a while of trial and error, but Dase and his doctor eventually figured out the correct dosage of the medication that would help alleviate pain without turning him into what he describes as "a vegetable."
Recently, however, his doctor, without a clear explanation, cut back his medication.
“It made such a difference; it was really bad,” he said. “I can literally only move around two to three hours a day. I used to be able to move three to four hours with a lot less pain.”
Dase believes state regulators are pressuring doctors to decrease the amount of opioid medications they’re prescribing.
After thousands of people died from heroin and opioid overdoses amid a national scourge, lawmakers in New Jersey have tackled the addiction crisis by reforming drug offenders through the Drug Court, providing recovery support to addicts, and cracking down on doctors who overprescribe opioids.
Last year, the state changed the the rules for prescribing pain medication, limiting the initial supply to just five days.
The state last year also joined a growing number of states and localities that have sued pharmaceutical companies, accusing them of creating and fueling the addiction crisis by irresponsibly promoting painkillers.
But chronic pain sufferers have warned that treating all patients like potential addicts is a mistake.
"Why would the government say we’re going to put you in more pain because there’s too many people out there using these drugs, so now you’re going to suffer because we’re trying to stop this?” Dase said.
“I think the regulating they’re doing is hurting the actual patients. There’s got to be a better way for them to see who are the abusers and who are the actual patients.”
Dase is now required to take blood tests on a regular basis to see if other medications are in his system.
On several occasions, the test has come back with a false positive, indicating he had something in his system that wasn’t there. He had to request a second blood test to prove the first was incorrect, otherwise he would have had his pain medication cut back even more.
Dase said doctors should be able to look at patient records and be able to understand who needs this medication and who may be abusing it.
“People like me need something that works, and if we’ve found something that works, we’re not asking for more than what works.”
More From 94.3 The Point